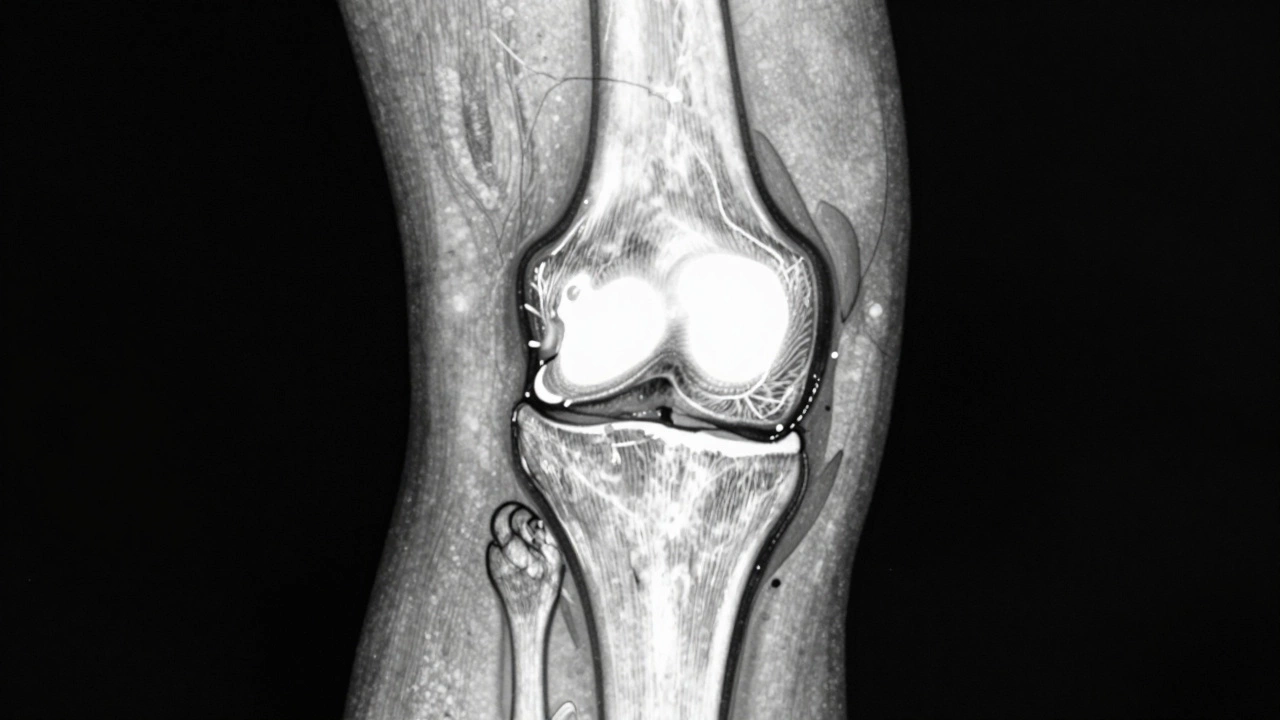
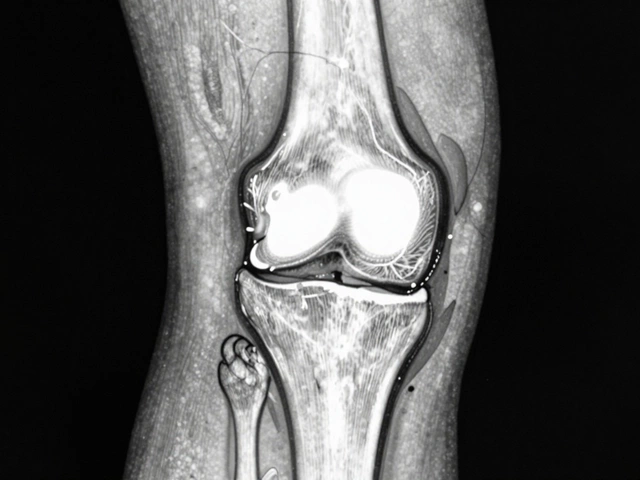
When your knee aches every morning or your fingers feel stiff after washing dishes, you might wonder: Can you see arthritis on an MRI? The short answer is yes-but not always in the way you expect. An MRI doesn’t show arthritis like a broken bone. It shows the hidden damage behind the pain. And that’s why doctors turn to it when X-rays aren’t enough.
What an MRI Actually Captures in Arthritis
Arthritis isn’t just "wear and tear." It’s inflammation, cartilage loss, bone changes, and swelling in the soft tissues around the joint. An X-ray can show bone spurs or narrowing between bones, but it misses the early signs. That’s where MRI comes in. It uses powerful magnets and radio waves to create detailed images of soft tissues, ligaments, tendons, and fluid buildup.
For example, in osteoarthritis, an MRI can reveal:
- Thinning or complete loss of cartilage in specific areas of the knee or hip
- Small bone bruises (bone marrow lesions) that cause sharp pain
- Fluid trapped in the joint space, indicating active inflammation
- Tears in the meniscus (in the knee) or labrum (in the shoulder or hip)
In rheumatoid arthritis, the MRI picks up even more:
- Inflammation of the synovial membrane (synovitis)-the lining that gets attacked by the immune system
- Erosions in the bone before they’re visible on X-ray
- Tendon inflammation or rupture, like in the wrist or ankle
These details matter because they help doctors decide if you need medication, physical therapy, or surgery-not just based on how much pain you feel, but on what’s actually happening inside.
When Is an MRI Needed for Arthritis?
Not everyone with joint pain needs an MRI. In fact, most cases of mild osteoarthritis are diagnosed based on symptoms and X-rays alone. But there are clear situations where an MRI becomes necessary:
- You have pain that doesn’t match your X-ray results. For instance, your X-ray shows minor changes, but you can barely walk.
- Your doctor suspects rheumatoid arthritis or another autoimmune form, and early treatment is critical.
- You’ve had a sports injury or fall, and you’re not improving after weeks of rest.
- There’s swelling, warmth, or redness around the joint that suggests active inflammation.
- You’re being considered for joint replacement surgery, and the surgeon needs to map out the exact damage.
One real-world case from a London orthopedic clinic in 2024 involved a 52-year-old woman who had knee pain for two years. Her X-rays looked "mild," but her MRI showed full-thickness cartilage loss in the inner knee, a torn meniscus, and bone marrow swelling. That explained why walking even short distances felt unbearable. Without the MRI, she might have been told to just "live with it." Instead, she got targeted physical therapy and avoided surgery for over a year.
What Arthritis Looks Like on an MRI Scan
Reading an MRI isn’t like reading a photograph. It’s like looking at layers of a cake-each slice shows a different depth of the joint. Radiologists use three main types of MRI sequences to spot arthritis:
- T2-weighted images: These highlight fluid. If you see bright white areas around the joint, that’s often inflammation or excess synovial fluid.
- STIR (Short Tau Inversion Recovery): This suppresses fat signal and makes inflammation stand out even more. Bone marrow edema-often invisible on X-rays-glows brightly here.
- Gradient echo or fat-suppressed images: These show cartilage thickness and defects clearly. A healthy cartilage layer looks smooth and dark. A damaged one looks thin, uneven, or missing entirely.
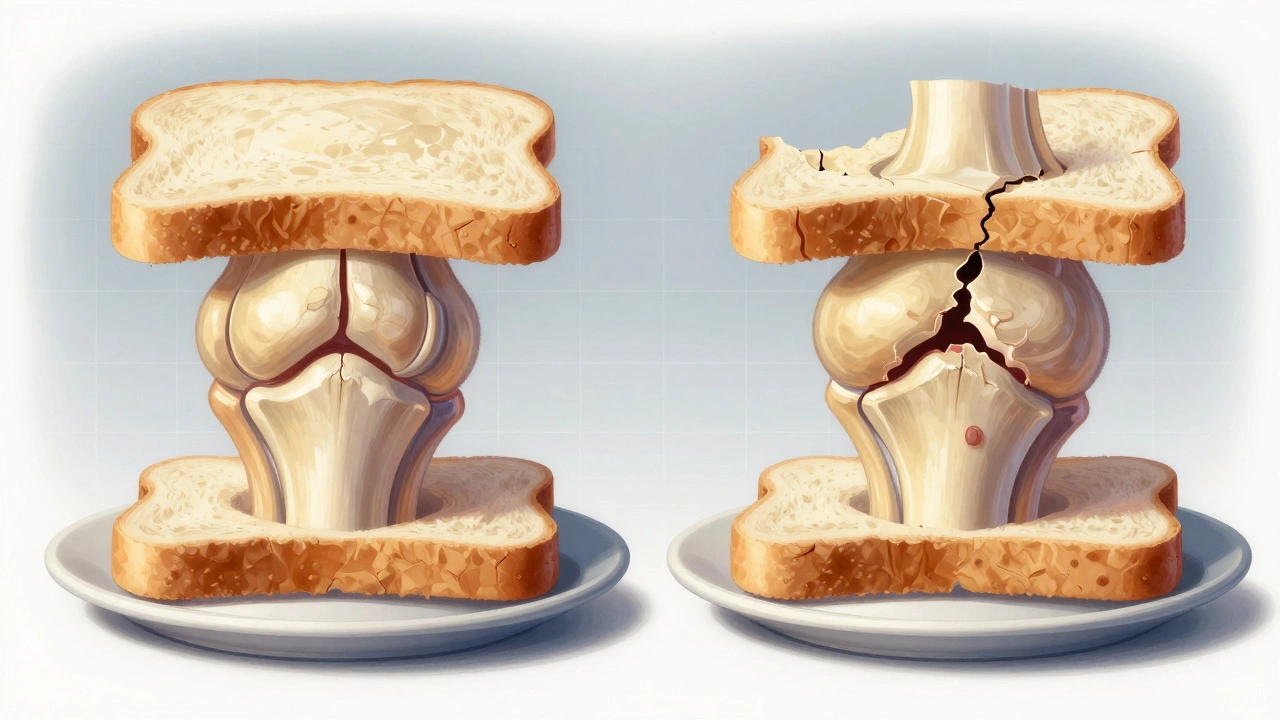
Imagine the knee joint as a sandwich. The cartilage is the bread, the meniscus is the filling, and the bone is the plate underneath. On an MRI, if the bread is crumbling or missing in spots, and the filling is swollen or torn, that’s arthritis in action. The plate might also show tiny dents or bruises where the cartilage used to cushion it.
How MRI Compares to Other Imaging Tests
It’s easy to assume MRI is always the best test. But that’s not true. Each tool has its place:
| Test | Best For | Shows Soft Tissue? | Shows Early Damage? | Cost (UK Estimate) |
|---|---|---|---|---|
| X-ray | Basic bone changes, joint space narrowing | No | No | £50-£120 |
| Ultrasound | Joint fluid, tendon inflammation, real-time movement | Yes (limited) | Yes (in some cases) | £100-£200 |
| CT Scan | Bone detail, complex fractures | Poor | No | £200-£400 |
| MRI | Early cartilage loss, bone marrow lesions, ligament/tendon damage | Yes (excellent) | Yes (best available) | £300-£600 |
Ultrasound is cheaper and great for checking fluid or tendon issues in real time-but it can’t see deep inside bones. CT scans give sharp bone images but expose you to radiation and miss soft tissue. MRI wins when the goal is to catch arthritis early, before the joint is too damaged.
Limitations and Misconceptions
Just because an MRI shows damage doesn’t mean it’s the cause of your pain. A 2023 study in the British Journal of Sports Medicine found that 40% of people over 50 with no joint pain had MRI findings of cartilage loss or meniscus tears. That’s right-damage without symptoms.
So what does that mean? It means MRI results must be matched with your symptoms. A scan showing severe arthritis doesn’t automatically mean you need surgery. Some people with "terrible" scans feel fine. Others with "mild" scans are in agony.
Also, MRI can’t tell you if the arthritis is getting worse right now. It’s a snapshot, not a movie. To track progression, doctors often compare scans taken months or years apart.
What Happens After the MRI?
If your MRI confirms arthritis, your doctor will likely combine the results with:
- Your medical history
- Physical exam findings
- Lab tests (like blood markers for rheumatoid arthritis)
- Your daily activity levels
Treatment isn’t one-size-fits-all. For early osteoarthritis, it might mean weight management, strengthening exercises, or injections. For inflammatory arthritis, it could mean disease-modifying drugs like methotrexate or biologics. Surgery is only considered when pain is disabling and other options have failed.
One patient I spoke with-61, retired teacher, knee pain for four years-was told she needed a knee replacement after her MRI. But her pain only happened after long walks. Her doctor recommended a walking cane, custom insoles, and a 12-week strengthening program. Six months later, she was hiking again. The MRI showed damage, but it didn’t dictate her future.
Final Takeaway
Yes, you can see arthritis on an MRI-but seeing it doesn’t mean you’re doomed. It means you have information. And information lets you make smarter choices. Whether it’s changing how you move, starting medication, or delaying surgery, an MRI gives you a map of what’s happening inside. But the decision of what to do next? That’s still yours, guided by your doctor, not a scan.
Can an MRI detect arthritis before it shows on an X-ray?
Yes. MRI can spot early cartilage thinning, bone marrow swelling, and synovial inflammation months or even years before changes appear on an X-ray. This is especially helpful for rheumatoid arthritis and early osteoarthritis, where early treatment can slow progression.
Is an MRI painful or dangerous for arthritis patients?
No. An MRI is non-invasive and doesn’t use radiation. You lie still in a tunnel-like machine for 20-45 minutes. Some people feel claustrophobic or find the noise uncomfortable, but it’s not painful. If you have metal implants (like joint replacements), inform the technician-they’ll check if it’s safe.
Can you have arthritis even if your MRI looks normal?
Yes. In rare cases, especially with early-stage or inflammatory arthritis, MRI may not show clear signs yet. Blood tests, physical exams, and ultrasound might be needed. Pain without visible damage doesn’t mean it’s "all in your head"-it just means more tools are needed to diagnose.
How accurate is MRI for diagnosing arthritis?
MRI is one of the most accurate tools for detecting early joint damage, especially for cartilage, bone marrow, and soft tissue. Studies show it’s over 90% accurate in identifying cartilage loss and bone marrow lesions in the knee. However, accuracy depends on the scanner quality and the radiologist’s experience.
Will insurance cover an MRI for arthritis in the UK?
If you’re using the NHS, an MRI will be ordered by your GP or specialist if clinically needed, and there’s no cost to you. Private patients usually pay between £300 and £600 depending on the joint scanned and location. Most private health insurance plans cover MRI for arthritis if it’s deemed medically necessary.