Cancer Pain Stage Explorer
Select a stage to understand why pain occurs and what it typically feels like.
Localized Nerve Irritation
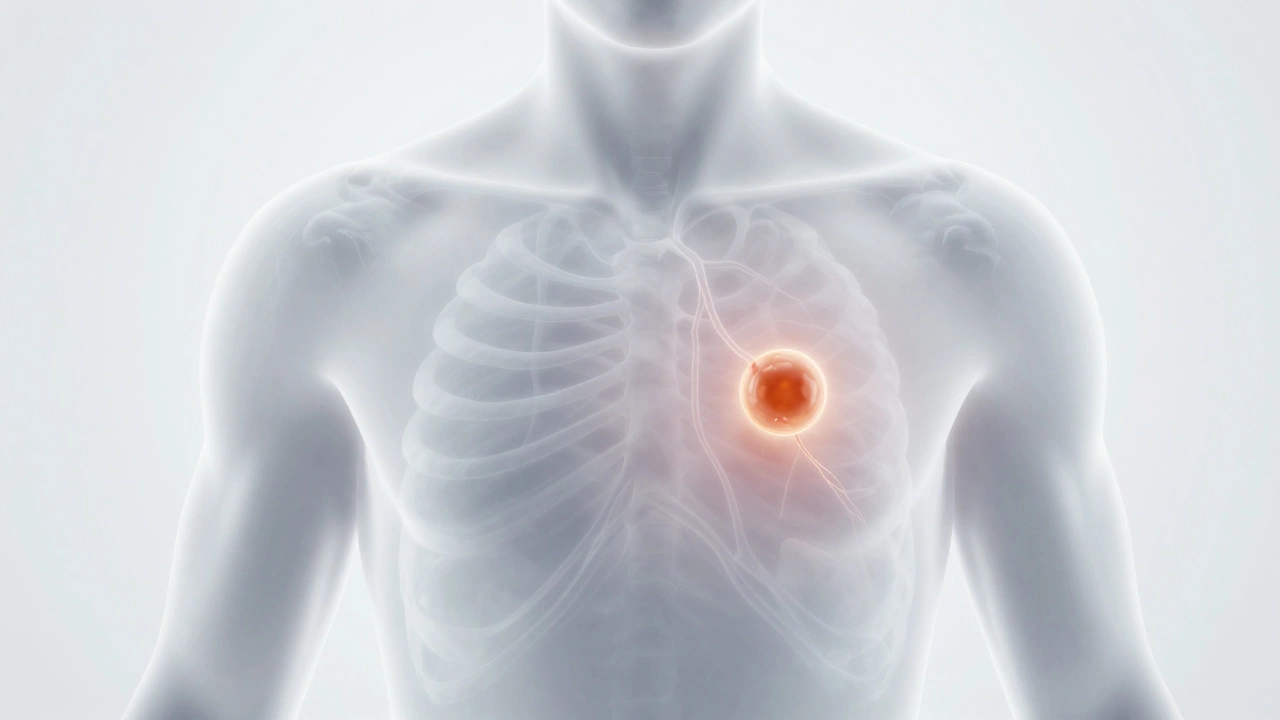
At this early stage, pain is often absent. Tumors are typically small clumps of cells. Pain only occurs if the tumor is located in an area with high nerve density or is pressing against a sensitive receptor.
For some, pain is a Day 1 symptom. For others, it doesn't show up until the very end. Understanding why this happens can help you spot the difference between a random ache and a signal that something is seriously wrong.
The Truth About Early Stage Pain
In many cases, Stage I Cancer is completely painless. Why? Because tumors usually start as small clumps of cells. Unless that clump is pressing on a nerve or sitting in a spot with lots of sensory receptors, your brain simply doesn't get a signal that anything is wrong. You might have a lung tumor the size of a grape, but since the lungs themselves don't have many pain receptors, you won't feel it until it hits the chest wall or causes a cough.
However, some cancers are "noisy" from the start. If a tumor grows in a place with high nerve density-like the skin or certain organs-you might feel discomfort even in the earliest phases. For example, someone with Basal Cell Carcinoma (a type of skin cancer) might feel tenderness or itching long before the cancer spreads. In these cases, pain isn't a sign of the cancer pain stages progressing, but rather a result of the tumor's specific location.
When Pain Becomes a Primary Symptom
As cancer moves into Stage II and Stage III, the "silent phase" usually ends. Pain at this point isn't usually caused by the cancer cells themselves, but by the space the tumor is taking up. Think of it like a crowd in a small room; eventually, people start getting pushed against the walls.
This is called "compression pain." When a tumor grows, it pushes against nearby organs, blood vessels, and nerves. If a tumor in the colon grows large enough to block the flow of waste, it causes cramping and sharp pain. If a brain tumor increases pressure inside the skull, it leads to those classic, splitting headaches. At this stage, the pain is often localized-you can point exactly to where it hurts.
Another common trigger in middle stages is inflammation. The body recognizes the tumor as a foreign object and sends immune cells to fight it. This creates swelling and redness, which puts more pressure on the surrounding tissue, leading to a dull, constant ache that doesn't go away with rest.
| Stage | Likelihood of Pain | Primary Cause of Discomfort | Typical Sensation |
|---|---|---|---|
| Stage I | Low | Localized nerve irritation | Mild tenderness or no feeling |
| Stage II | Moderate | Tissue compression | Dull ache, localized pressure |
| Stage III | High | Organ dysfunction/Blockage | Sharp, intermittent or constant pain |
| Stage IV | Very High | Metastasis to bone/organs | Deep bone pain, systemic aching |
The Shift in Stage IV: Metastatic Pain
When cancer reaches Stage IV, the pain often changes character. This is because the cancer has likely undergone Metastasis, meaning it has traveled from the original site to other parts of the body. The most common destination for metastatic pain is the bone.
Bone pain is notoriously difficult to manage. It's often described as a deep, boring ache that feels like it's coming from the inside of the skeleton. This happens because cancer cells destroy the bone matrix and trigger the release of chemicals that sensitize the nerves. If the cancer spreads to the spine, it can cause "cord compression," which can lead to sudden, severe pain or even paralysis if not treated immediately.
At this advanced stage, pain isn't just coming from the tumor anymore. It's often a mix of three things: the disease itself, the side effects of Chemotherapy (like neuropathy), and the emotional toll of the diagnosis. This is why the focus often shifts toward Palliative Care, which is specialized medical care focused on providing relief from the symptoms and stress of a serious illness.

Treatment-Induced Pain vs. Disease Pain
It's a bit of a cruel irony that the tools we use to kill cancer often cause their own kind of pain. You might feel a surge of discomfort even if your cancer is shrinking. For instance, Radiation Therapy can cause skin burns or internal inflammation that feels like a deep bruise. Many patients experience "peripheral neuropathy" from chemo, which feels like electric shocks or burning in the fingertips and toes.
Distinguishing between the two is vital. Disease pain tells the doctor the tumor might be growing or moving. Treatment pain tells the doctor the medication is working (or is too strong). If you're tracking your pain, be specific. Don't just say "it hurts." Say "it's a burning sensation in my feet" or "it's a sharp pain in my lower back when I breathe." This specificity allows the medical team to adjust dosages or change the type of painkiller used.
Strategies for Managing Cancer Pain
Pain management isn't just about popping pills. It's a tiered approach. Doctors typically follow the "WHO Pain Ladder," starting with non-opioids and moving up to stronger medications only as needed. But there are other ways to take the edge off.
- Physical Therapy: Gentle movement can prevent joint stiffness and reduce the pressure caused by fluid buildup (edema).
- Nerve Blocks: For severe localized pain, doctors can inject an anesthetic directly into a nerve to "shut off" the pain signal.
- Integrative Therapies: Things like acupuncture or massage don't cure the cancer, but they can lower the brain's perception of pain by releasing endorphins.
- Psychological Support: Anxiety and depression actually lower your pain threshold. When you're stressed, your brain amplifies pain signals, making a 4/10 ache feel like an 8/10.

When to Call the Doctor Immediately
While some discomfort is expected, certain types of pain are red flags that require an emergency visit. If you experience sudden, severe back pain accompanied by numbness in your legs, it could be spinal cord compression. If you have a sudden, "worst headache of your life" sensation, it could indicate a brain metastasis causing high intracranial pressure.
Similarly, any pain accompanied by a high fever or sudden shortness of breath could mean a blood clot or a severe infection. Pain is a communication tool; when it changes suddenly or becomes unbearable, it's the body's way of saying the current management plan is no longer working.
Does pain always mean the cancer is spreading?
No. Pain can be caused by many things: inflammation, side effects of treatment, or simply the tumor pressing against a nerve. It does not automatically mean the cancer has moved to a new stage or spread to other organs.
Can cancer be painless even in Stage IV?
Yes, it is possible. Some patients with advanced cancer in the lungs or certain abdominal organs may feel very little pain until the disease affects the nervous system or creates a significant blockage. This is why regular screening is so important even when you feel great.
What is the difference between acute and chronic cancer pain?
Acute pain is sudden and usually short-term, like pain from a biopsy or a sudden blockage. Chronic pain is long-term, persisting for months, and is often caused by the tumor's steady growth or nerve damage (neuropathy).
Are opioids the only way to treat advanced cancer pain?
Definitely not. Doctors use a variety of tools, including NSAIDs, corticosteroids to reduce swelling, antidepressants for nerve pain, and palliative radiation to shrink tumors that are pressing on nerves.
Why does bone pain feel different from other types of cancer pain?
Bone pain is often described as "deep" because the cancer disrupts the internal structure of the bone and triggers a chemical response that keeps the nerves in a state of high alert, unlike the "surface" pain felt in skin or muscle.
Next Steps for Patients and Caregivers
If you're dealing with pain, the first step is to keep a pain diary. Note the time of day, the exact location, the type of feeling (stabbing, burning, aching), and what makes it better or worse. This data is gold for your oncologist.
Depending on your situation, your next move might be:
- Asking for a referral to a pain management specialist if your current meds aren't working.
- Discussing "palliative radiation" if a specific spot is causing unbearable pain.
- Exploring non-drug options like gentle yoga or mindfulness to help manage the emotional side of chronic pain.